Thank You to Our Heroes!
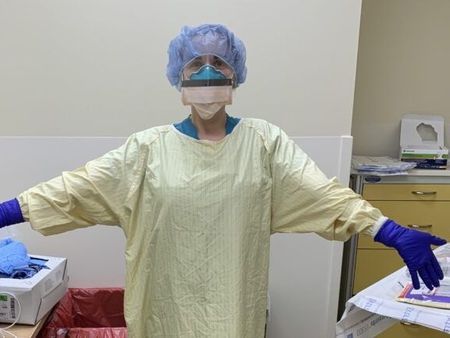
Stephanie Bandyk, ICU RN at Swedish Hospital in Seattle
Today we want to honor Stephanie Bandyk, ICU RN at the Swedish Hospital in Seattle, Washington. Here is her story as reported by MEGHANA KESHAVAN for STAT.
Stephanie Bandyk is on the front lines of the Covid-19 pandemic: A registered nurse who works in the intensive care unit of Seattle’s Swedish Hospital, she has helped treat some of the earliest patients infected with the novel coronavirus in the U.S. She has been working overnight shifts, from 7 p.m. to 7:30 a.m. in the state hardest hit by the new disease. There have been more than 1,000 cases of Covid-19 reported in Washington state, and at least 52 deaths.
In the most serious cases, the virulent pathogen has triggered severe pneumonia, and even multiple organ shutdown and death. Others in the Seattle area, as Bandyk points out, have had mild symptoms and have been able to self-treat at home.
STAT chatted with Bandyk about her experience in a Seattle ICU, as the coronavirus case count there steadily rises.
“The number of patients is just going to increase from here,” Bandyk said. “That’s just kind of how it is.”
The interview has been edited for clarity and length.
In recent days, the country and states have taken several aggressive measures to control the spread of coronavirus. What are your thoughts?
I think they’ve been reasonable. I think our initial response was too small, and it may have contributed to some of the spread. I think that it’s essential for people to listen now, and do their part in stopping the spread. I know that it is difficult for those not affected by this to fully understand, and to them this may seem overblown. But it is important.
Seattle was hit first, and hard. Did you have any preparation before Covid-19 arrived in Washington state?
Well, when Ebola happened, we went through practice drills. This has been very different. For this, we had a whole bunch of educators, and for the first couple days of it, educators were out on the floors. I work night shifts, so I don’t normally see these people, but they were there to help us out, and make sure that we were putting on everything appropriately.
It was a little confusing at first, but several days after we got our first case, they got more organized with it. They were having little in-services in the hospital before people would start their shift, to teach them how to don and doff all their protective equipment properly.
Things are changing almost daily, with what they want us to do and not do — but we’re trying to follow CDC guidelines for most of it.
How has Covid-19 testing been going in the Seattle area?
It was terrible at first — only the Department of Health was able to do it. It had a two-day turnaround time at first. Then, after the University of Washington stepped in, the turnaround time became just one day. Now, though, so many tests are being run that all of ours are going through LabCorp. The turnaround time had previously improved, but now it’s back to taking days.
We’re seeing reports that some Seattle health workers are making their own masks out of office supplies. Does your hospital have enough equipment?
In the ICU, we do. I think that situation applies more to health care workers that are in spots where they don’t really need masks, but want to protect themselves anyway. But for the areas that need the masks, they are there.
We do have some things that are in short supply, so we’ve been asked to reuse what we can. We can reuse N95 masks for a little while before we have to throw them out, and there are some cloth gowns that will get washed and come back to us.
But we’ve so far had enough personal protective equipment — it’s been pretty well-rationed. In terms of our N95 masks, if we used up the box, we’ve had to call our nursing supervisor to get another box. It’s all kept under lock and key, so people don’t take stuff home.
What sorts of patients are you treating?
All sorts. Mostly older people, and the most serious cases are the people with other comorbidities. But we’ve even had some 20-year-olds in critical care. In another hospital here in Washington, some children are being treated for Covid-19 as well. People think kids don’t get sick — but some of them do.
It’s important to note that in most of these coronavirus cases, however, most people don’t need to be in the hospital. I know a lot of people are freaked out, worrying they’ll end up in the ICU. A lot of people are able to deal with this at home.
What symptoms are the critical patients experiencing?
First, they’ve started out with just a dry cough. After that, they end up with shortness of breath, and high fevers — above 104. When the shortness of breath gets to be too much of an issue, that’s when patients tend to come to the hospital. You can only feel like that for so long before your body gets exhausted, and says “we can’t do this anymore.” So, at that point, we can see this on chest X-rays, and sometimes we have to intubate. Multiple organ shutdown, for some patients, comes later.
So what does your job as an ICU nurse entail?
I’m the nurse. So I do everything. (Laughs.)
I have respiratory therapists that I work with, and they help me out with the ventilator. Then there’s an ICU doctor that rounds the floor, and they’ll usually help me out with whatever I need, but mostly, they drive the care. They’ll figure out what antibiotic, or what antiviral, or whatever drug it is that a patient needs. From there, we watch labs, replace electrolytes, and basically make sure they don’t get worse.
It’s been kind of rough right now, because we can’t have as many people in the rooms as we normally would. Normally, ICU nurses take care of two patients at a time. For a while, we were limiting one Covid-19 patient per ICU nurse. But we’re back to our normal ratio again, because we’re getting more and more patients now. Last night, I had two patients.
And I’ve been doing OK, because my patients are doing all right — but it gets a little bit difficult when you’ve got patients that are really bad and getting worse, and you get stuck in a room. Thankfully, we’ve all been helping each other out, so all the patients have been getting the care that they need.
We have 16 beds on my unit, and five were positive Covid-19 patients. Four of them were rule-out patients that we’re waiting for lab tests to come back, and the rest were just normal ICU patients.
We actually have travel nurses that are here, now, to help us out with everything.
Is your hospital using experimental drugs, like Gilead’s antiviral remdesivir?
Remdesivir — yes, we’ve been doing that, if patients consent before getting the drug. As far as we’re concerned, giving out this drug has been very controlled. The pharmacy actually hand-delivers the remdesivir to you, and you have to hang the medication within four hours of them giving it to you.
Have you seen any critical patients recover yet?
I know at least one of my patients was discharged. Actually, his family sent our whole unit a bunch of pizza. There are people that are recovering, and getting out of the hospital. I just don’t think that there’s a lot of the recoveries that are being reported.
Not many American Covid-19 patients who’ve required critical care have spoken with the media yet. Do you have any thoughts as to why? And how are they doing?
Well, if these patients want to talk to somebody, they’ll want to talk with their family. Unless they’re imminently dying, there are no visitors allowed in the hospital. And even then, if they’re positive, then their entire family has to stay home in quarantine, anyway. It’s been challenging navigating that.
We’ve had to talk with lots of families who are unable to be at the bedside. They don’t know what’s going on with their loved ones — all they know is that their loved one is intubated, sedated, and Covid-positive.
But at least some patients are able to look at their phones, or use iPads. We’ve been loaning patients iPads, actually, so they can have more contact with the outside world — and their families. It’s hard to be isolated as a patient right now.
A lot of people are carefully following the news, and are very worried. Any advice?
Don’t rush into the hospitals. A lot are setting up hotlines for people to call. The issue with going to the ER: You’ll end up with people who probably don’t have it, mixed in with the people who do — so you run that risk of actually getting severely ill.
If you call, you can talk about your symptoms with a nurse over the phone, and they can help you decide whether to go to the hospital. Don’t bombard the ER.
And don’t panic.
This has all been very challenging. Are you concerned you’ll get ill? How are you holding up?
I’ve been fine. I’ve been working, and taking precautions. I think concern is a natural reaction, but I’m not anxious about it. I set up a clean area at the entrance to my home for me to change in and out of scrubs. I change and shower at work as well. I’m making sure to stay as healthy as I can, so that I can continue to care for others.
Some of my colleagues are nervous about working with Covid-19 patients, but a lot of people are just kind of happy to be here and to help out. We still have a lot of smiling faces, and jokes, and chocolate. I feel like people have been working really well together as a team, and help out where they see others who need help. And I think leadership has been really open and honest, and trying to get us all the information they can.
For now, I just go in and do what I can. I hope they get better, and go from there. If I can help somebody, I want to. That’s where I’m at.
Thank you Stephanie for your commitment, dedication, and compassion for your patients and communities.
If you have a story and pictures of a front line nurse you would like us to highlight on our website and social media, please email them to us at info@helphopehonor.org.
OUR DONORS
-
 KFA DJ Ken Ito
KFA DJ Ken Ito























